
Last updated: February 23, 2026
When you’re searching for the right assisted living residence for your loved one, you want a place that combines compassionate care with the latest innovations that keep residents safe, healthy, and connected. AI and technology integration in assisted living communities: 2026 innovations for better care are transforming how senior care services are delivered, offering unprecedented levels of personalization, safety monitoring, and quality of life improvements. These technological advances aren’t replacing the human touch—they’re enhancing it, giving compassionate caregivers better tools to provide dignified, responsive care.
Today’s tech-forward assisted living communities use smart sensors, artificial intelligence, and connected devices to monitor health in real time, predict potential problems before they become emergencies, and create personalized care plans that adapt to your loved one’s changing needs. This guide will help you understand what these innovations mean for your family and how to evaluate technology features when choosing a trusted care provider.
Key Takeaways
- AI-powered health monitoring tracks vital signs, movement patterns, and behavioral changes in real time, alerting staff to potential health issues before they become emergencies
- Smart home technology in resident rooms includes voice-activated controls, automated lighting, temperature adjustment, and fall detection systems that enhance safety and independence
- Predictive analytics help care teams anticipate resident needs, optimize medication schedules, and prevent falls through pattern recognition and risk assessment
- Wearable devices provide continuous health monitoring while respecting resident dignity and privacy, tracking heart rate, sleep quality, activity levels, and medication adherence
- Virtual care options connect residents with healthcare providers through telehealth, reducing unnecessary hospital transfers and improving access to specialists
- Family communication platforms offer real-time updates, video calls, and transparent care documentation that provide peace of mind
- Technology should enhance, not replace human interaction—the best facilities balance innovation with hands-on, compassionate care from trained staff
Quick Answer

AI and technology integration in assisted living communities in 2026 includes smart sensors that monitor health and safety, wearable devices that track vital signs, predictive AI that anticipates care needs, voice-activated smart home controls, telehealth platforms for virtual medical visits, and family communication apps. These innovations help prevent falls, detect early signs of illness, personalize care plans, and maintain resident independence while ensuring 24/7 safety monitoring. When evaluating facilities, look for communities that use technology to support—not replace—direct caregiver interaction and maintain the dignity and privacy of residents.
What AI and Technology Are Actually Used in Assisted Living Communities in 2026?
Assisted living communities in 2026 use a combination of artificial intelligence, smart home devices, wearable health monitors, and data analytics platforms to enhance daily care. The most common technologies include motion sensors that detect falls or unusual movement patterns, smart medication dispensers that ensure proper dosing, voice-activated room controls that help residents adjust lighting and temperature independently, and AI-powered health monitoring systems that analyze patterns in vital signs to predict potential health issues.
Core technologies you’ll find in tech-forward facilities:
- Environmental sensors mounted discreetly in rooms and common areas that monitor movement, detect falls, track sleep patterns, and identify changes in daily routines
- Wearable health devices including smartwatches and discrete sensors that track heart rate, blood pressure, oxygen levels, activity, and sleep quality
- AI care management platforms that analyze health data, medication schedules, and behavioral patterns to create personalized care recommendations
- Smart medication systems with automated dispensing, reminder alerts, and tracking to reduce medication errors
- Voice-activated assistants adapted for senior use, allowing residents to control room features, request help, or communicate with staff hands-free
- Telehealth equipment including video conferencing systems, remote examination tools, and digital health record integration
- Family communication portals providing secure access to care updates, activity photos, health reports, and direct messaging with staff
These technologies work together as an integrated system. For example, if a wearable device detects an irregular heartbeat, the AI platform alerts nursing staff immediately, while environmental sensors confirm the resident’s location and activity level, allowing for rapid, informed response.
Common mistake to avoid: Don’t assume more technology automatically means better care. The best communities use technology to support their staff, not replace them. Ask how technology enhances caregiver-resident relationships rather than reducing face-to-face interaction. Learn more about quality standards in our guide to assisted living residence performance metrics.
How Does AI Improve Safety and Fall Prevention in Assisted Living?
AI-powered fall prevention systems in 2026 use machine learning algorithms that analyze movement patterns, gait changes, and environmental factors to predict fall risk before incidents occur. These systems combine data from floor sensors, wearable devices, and video monitoring (with privacy protections) to identify residents at elevated risk and trigger preventive interventions.
How AI fall prevention works in practice:
- Baseline establishment – The system learns each resident’s normal movement patterns, walking speed, balance, and daily routines during the first few weeks
- Continuous monitoring – Sensors track changes in gait, hesitation before standing, increased nighttime bathroom trips, or other risk indicators
- Risk scoring – AI algorithms calculate a daily fall risk score based on multiple factors including medication changes, recent illness, and movement pattern shifts
- Preventive alerts – When risk scores rise, the system notifies care staff to implement interventions like additional assistance, physical therapy, or environmental modifications
- Immediate response – If a fall occurs, sensors detect the impact and unusual stillness, triggering instant alerts to staff with the exact location
Real-world benefits families report:
- Faster emergency response times (typically under 60 seconds from fall detection to staff arrival)
- Reduction in serious fall-related injuries through early intervention
- Greater resident independence because continuous monitoring allows more freedom of movement
- Peace of mind for families who receive notifications about incidents and responses
Modern fall prevention systems also integrate with fall prevention programs that include environmental modifications, exercise programs, and regular risk assessments.
Decision rule: Choose AI fall prevention if your loved one has a history of falls, mobility challenges, or conditions affecting balance. However, ensure the facility explains how they protect privacy and maintain dignity while using monitoring technology.
What Smart Home Features Enhance Daily Living for Residents?
Smart home technology in assisted living residences in 2026 focuses on voice-activated controls, automated environmental adjustments, and intuitive interfaces designed specifically for older adults. These features help residents maintain independence and control over their personal space while accommodating physical or cognitive limitations.
Common smart home features in resident rooms:
| Technology | Function | Benefit for Residents |
|---|---|---|
| Voice assistants | Control lights, temperature, blinds, TV, and music through voice commands | Maintains independence for residents with limited mobility or vision |
| Smart lighting | Automated nighttime pathway lighting, gradual wake-up lighting, motion-activated bathroom lights | Reduces fall risk during nighttime bathroom trips |
| Temperature control | Personalized climate settings that adjust based on time of day and preferences | Improves comfort and sleep quality |
| Emergency call systems | Voice-activated or wearable emergency buttons with two-way communication | Faster help response without needing to reach a call button |
| Automated blinds/curtains | Scheduled opening/closing or voice control | Easier room darkening for sleep or opening for natural light |
| Smart door locks | Keyless entry with codes or cards, automatic locking, staff access logging | Enhanced security while allowing resident control |
| Medication reminders | Visual and audio alerts with confirmation tracking | Better medication adherence and reduced errors |
Personalization capabilities:
The best systems learn individual preferences over time. For example, if your mother always lowers the temperature and dims the lights at 9 PM, the system will begin doing this automatically while still allowing manual override. This predictive personalization helps residents feel at home while reducing the cognitive load of managing multiple devices.
Important consideration: Smart home features should be optional and customizable. Some residents embrace technology enthusiastically, while others prefer traditional controls. Quality facilities offer both options and provide patient training for residents who want to use smart features.
Edge case: For residents with dementia or cognitive impairment, smart home systems can be configured with simplified controls or fully automated settings that maintain comfort and safety without requiring resident interaction. Families can often adjust settings remotely through secure portals.
How Do Wearable Devices Monitor Health Without Compromising Dignity?
Wearable health monitoring devices in 2026 have evolved to be discreet, comfortable, and respectful of resident privacy and dignity. Modern wearables look like regular watches, jewelry, or clothing accessories while continuously tracking vital health metrics and transmitting data to care teams.
What wearables monitor in assisted living settings:
- Cardiovascular health: Heart rate, heart rhythm irregularities (like atrial fibrillation), blood pressure trends
- Respiratory function: Breathing rate, oxygen saturation, sleep apnea indicators
- Activity and mobility: Steps taken, time spent sitting vs. moving, exercise completion
- Sleep quality: Sleep duration, restlessness, time spent in different sleep stages
- Body temperature: Continuous monitoring that can detect fever or infection early
- Medication adherence: Confirmation when medications are taken (through smart pill bottles or ingestible sensors)
- Hydration status: Advanced devices can estimate hydration levels through bioimpedance
Privacy and dignity protections:
Reputable facilities implement strict protocols around wearable data. Health information is encrypted, accessed only by authorized care staff, and used solely for care purposes. Residents (or their healthcare decision-makers) must provide informed consent before monitoring begins. Many facilities allow residents to remove devices during private activities like bathing, with systems designed to distinguish intentional removal from emergencies.
Choose wearables if: Your loved one has chronic conditions requiring close monitoring (heart disease, diabetes, COPD), takes multiple medications, or has experienced recent health changes. Wearables provide continuous oversight without the intrusion of frequent vital sign checks.
Avoid or question if: The facility cannot clearly explain their data privacy policies, doesn’t offer opt-out options for certain monitoring features, or uses wearables as a substitute for regular in-person health assessments by trained staff.
The technology works best when integrated with comprehensive personalized care plans that address the whole person, not just data points.
What Role Does Predictive AI Play in Personalized Care Planning?
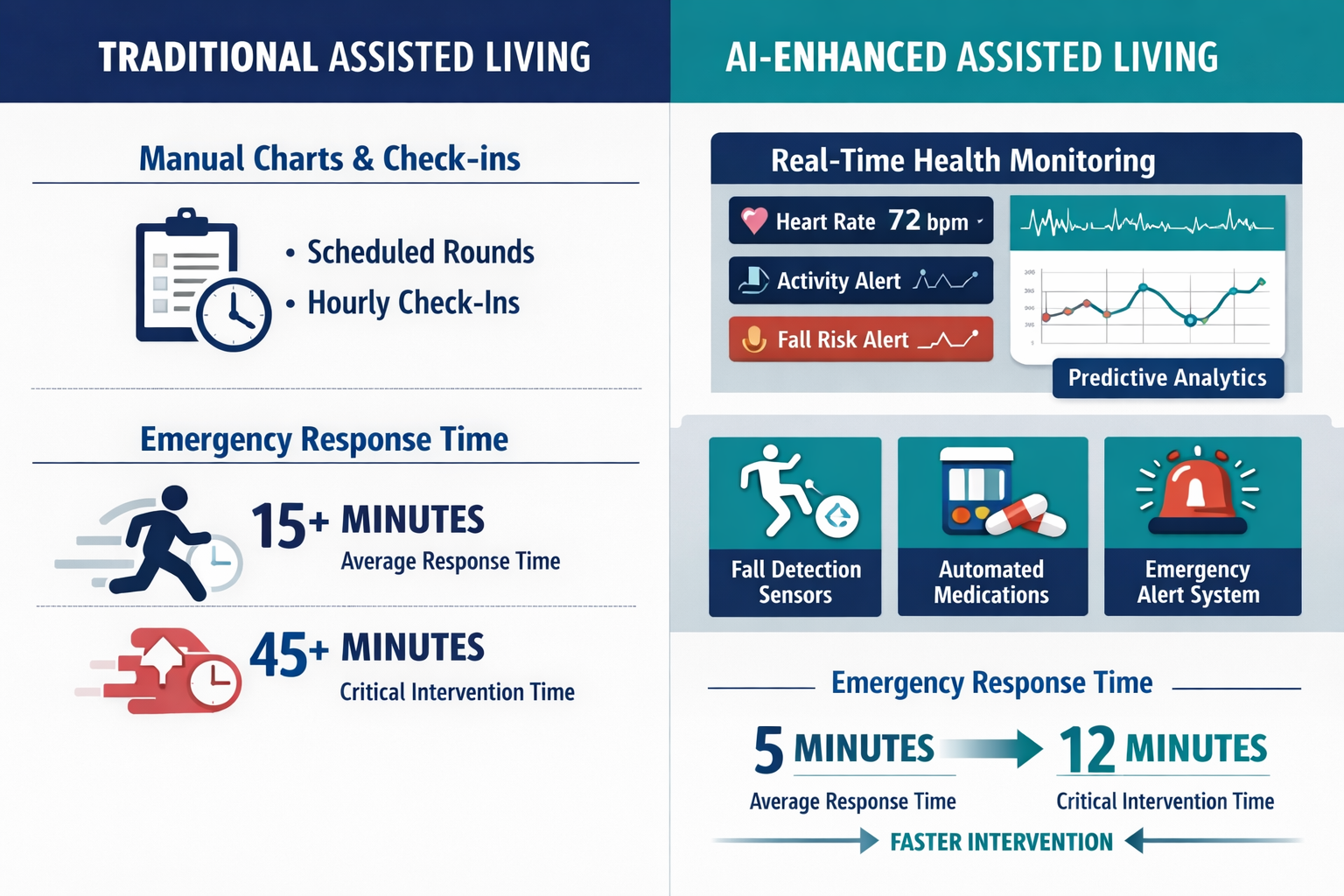
Predictive AI in assisted living analyzes patterns in health data, behavior, medication responses, and environmental factors to anticipate resident needs and optimize care delivery. These systems help care teams move from reactive to proactive care by identifying potential health issues days or weeks before they become acute problems.
How predictive AI enhances care planning:
Early illness detection – AI algorithms can identify subtle changes in vital signs, activity levels, or eating patterns that may indicate developing infections, heart problems, or other health issues before obvious symptoms appear. For example, a slight increase in resting heart rate combined with reduced activity might signal an infection 2-3 days before fever develops.
Medication optimization – By analyzing how individual residents respond to medications over time, AI can help physicians fine-tune dosages, timing, and combinations to maximize effectiveness while minimizing side effects. This is particularly valuable for residents taking multiple medications.
Behavioral health insights – For residents with dementia or other cognitive conditions, AI can identify triggers for agitation, confusion, or behavioral changes by correlating incidents with time of day, activities, visitors, or environmental factors. Care teams can then adjust routines to prevent distressing episodes.
Personalized activity recommendations – AI systems suggest activities, social events, or therapies based on individual interests, physical capabilities, and mood patterns. If the system notices your father is more engaged in the morning, it might recommend scheduling his favorite activities then.
Care plan adjustments – Rather than waiting for quarterly care plan reviews, AI provides continuous recommendations for care plan updates based on changing needs, allowing more responsive, individualized care.
Practical example:
Mrs. Johnson, an 82-year-old resident with diabetes and heart disease, wears a health monitoring device. The AI system notices her blood sugar levels are trending slightly higher in the afternoons and her activity level has decreased by 15% over two weeks. It alerts the care team, who discover she’s been skipping her afternoon walks due to foot discomfort. They arrange a podiatry visit, adjust her activity schedule, and modify her afternoon snack timing. A potential diabetic episode is prevented before it requires emergency intervention.
Critical point: Predictive AI should inform human decision-making, not replace it. The best facilities use AI recommendations as one input in care planning, combined with direct observation, resident preferences, family input, and clinical judgment from experienced caregivers.
How Does Technology Improve Communication Between Families and Care Teams?
Family communication technology in 2026 provides unprecedented transparency and connection between loved ones, residents, and care teams. Modern platforms offer real-time updates, secure messaging, video calls, and comprehensive care documentation accessible from smartphones or computers.
Key features of family communication platforms:
- Daily activity updates with photos showing your loved one participating in activities, meals, or social events
- Health status dashboards displaying vital signs, medication administration, sleep quality, and activity levels (with resident consent)
- Secure messaging allowing direct communication with care coordinators, nurses, and administrators
- Video calling with easy-to-use interfaces that residents can answer with a single touch or voice command
- Care plan access where families can review current care plans, upcoming appointments, and recent assessments
- Incident reporting with immediate notifications if falls, health changes, or other significant events occur
- Billing and administrative tools for reviewing charges, making payments, and accessing documents
- Appointment scheduling for family visits, care conferences, or external medical appointments
Benefits families consistently report:
Reduced anxiety – Knowing you can check in anytime and see real-time updates provides tremendous peace of mind, especially for adult children who live far away or have demanding work schedules.
Better advocacy – Access to detailed health information helps families ask informed questions during medical appointments and advocate effectively for their loved one’s needs.
Maintained connection – Easy video calling helps residents stay connected with grandchildren, friends, and extended family, reducing isolation and supporting emotional well-being.
Transparency builds trust – When facilities share comprehensive information openly, families feel more confident in the quality of care being provided.
Important consideration: While technology enables connection, it shouldn’t replace in-person visits. The best facilities encourage regular family involvement and use technology to supplement, not substitute for, face-to-face time. Additionally, facilities should respect resident privacy by requiring resident consent before sharing certain information with family members.
Red flag: Be cautious if a facility resists transparency or provides only limited, filtered information through their platform. Quality communities embrace open communication because they’re confident in their care delivery.
For more information on how facilities maintain open communication, see our guide on resident advocacy programs.
What Are the Benefits and Limitations of Telehealth in Assisted Living?
Telehealth services in assisted living communities allow residents to consult with physicians, specialists, mental health professionals, and therapists through video conferencing without leaving the facility. In 2026, most tech-forward communities have dedicated telehealth equipment and staff trained to facilitate virtual appointments.
Primary benefits of telehealth:
Reduced hospital transfers – Many minor health concerns can be addressed through virtual consultations, avoiding stressful and potentially risky trips to emergency rooms or urgent care facilities. This is especially valuable for residents with mobility challenges or those who become confused in unfamiliar environments.
Access to specialists – Residents can consult with cardiologists, endocrinologists, psychiatrists, and other specialists who may not be locally available, improving care quality without travel burdens.
Faster intervention – When health concerns arise, telehealth appointments can often be scheduled within hours rather than days, allowing quicker diagnosis and treatment.
Continuity of care – Residents can continue seeing their long-time physicians even after moving to assisted living, maintaining important relationships and medical history continuity.
Family participation – Family members can join telehealth appointments remotely, staying involved in healthcare decisions even when they can’t be physically present.
Cost savings – Virtual visits typically cost less than in-person appointments and eliminate transportation expenses.
Limitations and situations requiring in-person care:
- Physical examinations – Telehealth cannot replace hands-on physical exams, though some facilities have nurses who can perform examinations under physician video guidance
- Diagnostic testing – Lab work, imaging, and other tests still require in-person visits to medical facilities
- Emergency situations – Serious symptoms like chest pain, stroke signs, or severe injuries require immediate emergency room care
- Technology barriers – Some residents struggle with video technology, though staff assistance usually resolves this
- Relationship building – Some residents and physicians prefer in-person visits for building therapeutic relationships
Best practice approach: Telehealth works best as part of a hybrid care model that combines virtual visits for routine follow-ups, minor concerns, and specialist consultations with in-person visits for comprehensive exams, emergencies, and situations requiring hands-on care.
Decision rule: Telehealth is particularly valuable if your loved one has multiple chronic conditions requiring frequent specialist monitoring, has difficulty with transportation, or benefits from family participation in medical appointments when you live far away.
How Should Families Evaluate Technology When Touring Assisted Living Communities?
When visiting potential assisted living residences, you’ll want to assess not just what technology they have, but how effectively they use it to enhance care and quality of life. The most advanced systems mean little if staff aren’t properly trained or if technology creates barriers rather than solutions.
Questions to ask during facility tours:
About safety and monitoring:
- What fall detection and prevention systems do you use, and how quickly do staff typically respond to alerts?
- How do you balance safety monitoring with resident privacy and dignity?
- Can residents opt out of certain monitoring technologies while still receiving quality care?
- What happens if a wearable device malfunctions or a resident refuses to wear it?
About care coordination:
- How does technology help staff coordinate care across shifts and departments?
- Can you show me an example of how health data informs care planning? (Ask for a demonstration)
- How do you ensure staff actually review and act on AI-generated alerts and recommendations?
- What’s your protocol when technology identifies a potential health concern?
About family communication:
- What family portal or app do you use, and can I see a demo?
- How frequently are updates posted, and what type of information is shared?
- Can I communicate directly with my loved one’s care team through the platform?
- How do you handle technical issues or family members who aren’t tech-savvy?
About resident experience:
- How do you train residents to use smart home features and other technologies?
- What happens if a resident doesn’t want to use technology in their room?
- Can residents (or families) customize technology settings based on preferences?
- Do you have examples of residents who’ve benefited from specific technologies?
About staff training and integration:
- How are staff members trained on your technology systems?
- What’s your staff-to-resident ratio, and has technology changed that ratio?
- How do you prevent technology from reducing face-to-face interaction time?
- Who handles technical support when systems malfunction?
Red flags to watch for:
- Staff who can’t explain how technology works or seem unfamiliar with systems
- Technology that appears unused or poorly maintained
- Facilities that emphasize technology but have low staffing levels
- Inability or unwillingness to demonstrate systems during your tour
- Vague answers about data privacy and security
- Technology that seems to create more work for staff rather than supporting efficiency
- No backup plans for when technology fails
Green flags that indicate effective technology integration:
- Staff enthusiastically explain how technology helps them provide better care
- Residents are observed actually using smart features in their rooms
- Clear, written policies about data privacy, consent, and technology use
- Technology that’s integrated seamlessly into care routines, not treated as separate
- Regular technology training for staff and optional training for residents
- Balance between high-tech monitoring and high-touch personal interaction
Practical tip: Ask to speak with current residents or families about their experiences with the facility’s technology. Their real-world insights will be more valuable than marketing materials.
For additional evaluation criteria, review our guide on assisted living residence trial stay programs, which can help you assess technology and other features firsthand.
What Privacy and Security Protections Should Be in Place?
With extensive health monitoring and data collection, privacy and security protections are critical considerations when evaluating AI and technology integration in assisted living communities. Reputable facilities implement comprehensive safeguards to protect resident information and maintain dignity.
Essential privacy protections:
Informed consent – Residents (or their legal healthcare decision-makers) should provide explicit consent before any monitoring begins. Consent forms should clearly explain what data is collected, how it’s used, who has access, and how long it’s retained.
Data encryption – All health information should be encrypted both in transit (when transmitted between devices) and at rest (when stored in databases). This prevents unauthorized access even if systems are breached.
Access controls – Only staff members with direct care responsibilities should access resident health data. Systems should log every access instance, creating accountability and allowing audit trails.
Video monitoring limitations – If facilities use video monitoring (increasingly rare due to privacy concerns), cameras should never be placed in bathrooms, bedrooms, or other private spaces. When used in common areas, clear signage should notify residents and visitors.
Data minimization – Facilities should collect only data necessary for care purposes, not gather excessive information for other uses.
Retention policies – Clear policies should govern how long data is kept and how it’s securely destroyed when no longer needed.
Third-party vendor agreements – Technology vendors should sign business associate agreements (required under HIPAA) committing to protect resident information.
Security measures to expect:
- Regular security audits and vulnerability testing
- Staff training on privacy regulations and data handling
- Secure, password-protected family portals with multi-factor authentication
- Incident response plans for data breaches or security failures
- Compliance with HIPAA, state privacy laws, and industry standards
- Physical security for servers and devices storing resident information
Questions about privacy to ask:
- How do you comply with HIPAA and state privacy regulations?
- Who has access to my loved one’s health data, and how is access logged?
- Can we review and correct information in my loved one’s digital health record?
- What happens to health data if my loved one moves to a different facility?
- Have you experienced any data breaches, and if so, how were they handled?
- How do you protect against cybersecurity threats?
Your rights regarding data:
Under HIPAA and most state laws, you (or your loved one) have the right to access health records, request corrections to inaccurate information, receive an accounting of disclosures, and file complaints if privacy is violated. Quality facilities will explain these rights clearly and honor them promptly.
Important note: Privacy protections should never compromise safety. The best facilities find the right balance—using technology to monitor health and prevent emergencies while respecting dignity and maintaining appropriate boundaries.
For more information on regulatory compliance, see our guide on medication error reporting rules.
How Much Does Technology-Enhanced Assisted Living Cost?

Technology-enhanced assisted living communities typically charge monthly fees that range from 10-25% higher than traditional facilities, though this varies significantly by location, level of technology integration, and services included. In 2026, the national average for tech-forward assisted living ranges from $5,500 to $8,000 per month, compared to $4,500 to $6,500 for traditional communities.
What influences technology-related costs:
Infrastructure investment – Facilities with comprehensive smart home systems, extensive sensor networks, and advanced AI platforms have higher operational costs that are reflected in monthly fees.
Staff training – Ongoing training to keep staff current with technology systems adds to operational expenses.
Technology maintenance and updates – Software subscriptions, hardware replacement, cybersecurity measures, and system upgrades create ongoing costs.
Level of monitoring – More intensive health monitoring with wearables and real-time analytics typically costs more than basic safety monitoring.
Family communication platforms – Some facilities include family portal access in base fees, while others charge separately for premium features.
Telehealth services – Virtual care access may be included or offered as an add-on service.
Typical pricing structures:
- Base monthly fee covering room, meals, basic care services, and standard technology features (safety monitoring, emergency call systems)
- Care level fees that increase with higher care needs, often informed by technology-based assessments
- Technology package add-ons for enhanced monitoring, wearable devices, or advanced smart home features
- One-time technology setup fees ranging from $500-$2,000 for room customization and system configuration
Cost-benefit considerations:
While technology-enhanced care costs more upfront, it may provide value through:
- Reduced hospitalizations – Early detection and intervention can prevent costly emergency room visits and hospital stays
- Better medication management – Fewer medication errors and optimized prescriptions may reduce overall healthcare costs
- Extended independence – Technology that supports independence may delay the need for more intensive (and expensive) nursing home care
- Family peace of mind – The value of reduced worry and easier communication, while not financial, is significant for many families
Financial planning tips:
Review your loved one’s long-term care insurance policy to see if it covers technology-enhanced assisted living. Some policies cover these costs if the technology is deemed medically necessary. Additionally, consider the total cost of care, not just monthly fees. A facility with higher base costs but fewer hospitalizations and better health outcomes may be more economical overall.
For comprehensive financial planning guidance, see our assisted living residence financial planning timeline.
Decision rule: Choose technology-enhanced care if your loved one has complex health needs, a history of falls or emergencies, multiple chronic conditions, or if you live far away and value detailed remote monitoring. Consider traditional care if your loved one is relatively healthy, prefers minimal technology, or if budget constraints make higher monthly fees unsustainable.
What Does the Future Hold for AI and Technology in Senior Care?
Looking beyond 2026, AI and technology integration in assisted living communities will continue evolving toward more sophisticated, personalized, and unobtrusive systems that enhance both care quality and resident autonomy.
Emerging technologies on the horizon:
Advanced robotics – Robots that assist with mobility, deliver medications, provide companionship, and help with daily tasks are becoming more capable and affordable. These won’t replace human caregivers but will handle routine tasks, freeing staff for more meaningful interactions.
Virtual reality therapy – VR is showing promise for pain management, cognitive stimulation, reminiscence therapy for dementia patients, and virtual travel experiences that enhance quality of life for residents with limited mobility.
Genomic-based care – Personalized medicine based on genetic profiles will allow more precise medication selection, disease risk prediction, and tailored nutrition and exercise programs.
Brain-computer interfaces – For residents with severe mobility limitations or communication difficulties, emerging interfaces may allow control of devices and communication through thought patterns.
Enhanced AI diagnostics – AI systems are becoming increasingly accurate at detecting diseases from voice patterns, gait analysis, and other subtle indicators, potentially identifying conditions like Parkinson’s or Alzheimer’s years earlier.
Social connection AI – Advanced AI companions that engage in meaningful conversation, remember personal histories, and provide emotional support are improving rapidly, though they’ll complement rather than replace human interaction.
Ambient monitoring – Future systems will monitor health through completely passive means—analyzing breathing patterns through mattress sensors, detecting infections through air quality sensors, or assessing nutrition through smart plates—eliminating the need for wearables.
Trends shaping the future:
Aging in place with technology – Advanced home care services technology may allow more seniors to remain in their own homes longer, with assisted living serving those with more complex needs.
Integration across care settings – Better data sharing between assisted living, hospitals, physicians, and home care services will create seamless care transitions.
Resident-controlled technology – Future systems will give residents more control over their care data, privacy settings, and technology preferences.
Equity and access – As technology becomes more affordable, it will spread beyond premium facilities to serve residents across income levels.
Ethical frameworks – The industry is developing clearer ethical guidelines around AI decision-making, data use, and the appropriate balance between monitoring and privacy.
What this means for families:
Technology will continue making assisted living safer, more personalized, and more transparent. However, the fundamental need for compassionate human care will never change. The best facilities will always be those that use technology to enhance—not replace—the relationships between caregivers, residents, and families.
When planning for your loved one’s future care needs, consider facilities that demonstrate both technological sophistication and a commitment to person-centered care. The communities that thrive will be those that master this balance.
Frequently Asked Questions
Will technology replace human caregivers in assisted living?
No, technology enhances caregiver capabilities but cannot replace human compassion, judgment, and personal connection. AI and smart devices handle monitoring, data analysis, and routine tasks, allowing caregivers to spend more time on direct resident interaction, emotional support, and complex care decisions that require human empathy and expertise.
How do assisted living communities protect resident privacy with all this monitoring?
Reputable facilities encrypt all health data, limit access to authorized care staff only, obtain informed consent before monitoring begins, never use cameras in private spaces like bedrooms or bathrooms, and comply with HIPAA regulations. Residents can typically opt out of certain monitoring features while still receiving quality care.
What happens if the technology fails or malfunctions?
Quality facilities have backup systems and protocols for technology failures. Staff are trained to provide care without technology if needed, emergency call systems have battery backups, and critical data is backed up regularly. Facilities should have 24/7 technical support and maintenance contracts with vendors to address issues quickly.
Can my loved one who isn’t tech-savvy still benefit from these innovations?
Yes, most monitoring and AI systems work passively in the background without requiring resident interaction. Smart home features can be fully automated based on preferences, and staff assist with any technology that does require resident participation. The benefits of health monitoring, fall detection, and improved care coordination don’t depend on the resident being tech-savvy.
How do I know if a facility’s technology actually works or is just marketing?
Ask for demonstrations during your tour, request data on outcomes like fall response times or hospital readmission rates, speak with current residents and families about their experiences, and observe whether staff actually use and understand the technology. Check online reviews and state inspection reports for insights into care quality.
Will my loved one’s health information be sold to third parties?
Reputable facilities never sell resident health information. HIPAA regulations strictly prohibit sharing protected health information without consent. Ask facilities directly about their data use policies and review privacy notices carefully. Any facility that cannot clearly guarantee they won’t sell data should be avoided.
How often should assisted living technology be updated?
Software should be updated regularly (often monthly) for security patches and feature improvements. Hardware like sensors and wearables typically has a 3-5 year replacement cycle. Facilities should have technology refresh plans and budgets to avoid operating on outdated systems that may have security vulnerabilities or reduced effectiveness.
Can I access my loved one’s health data remotely?
Most tech-forward facilities provide family portals or apps that allow authorized family members to view health data, activity updates, and care notes remotely. Access requires resident consent (or healthcare power of attorney if the resident cannot provide consent) and secure login credentials. The level of detail shared varies by facility.
What if my loved one has dementia and can’t consent to monitoring?
If your loved one has been declared legally incapable of making healthcare decisions, their designated healthcare power of attorney or legal guardian can provide consent for monitoring and technology use. Facilities should still explain technology to residents in terms they can understand and respect their preferences when possible, even with cognitive impairment.
Are there assisted living communities that offer traditional care without extensive technology?
Yes, many excellent assisted living communities provide high-quality care with minimal technology integration, focusing instead on high staff-to-resident ratios and hands-on care. Technology-enhanced care isn’t right for everyone, and you should choose based on your loved one’s needs, preferences, and your family’s priorities.
How do wearable devices handle bathing and water exposure?
Most modern wearable health devices are water-resistant and can be worn during bathing. However, some facilities allow residents to remove devices during bathing for comfort and privacy, with systems designed to recognize scheduled removal as normal rather than triggering alerts. Ask about specific policies during your facility tour.
What training do staff receive on using AI and technology systems?
Quality facilities provide comprehensive initial training when technology is implemented, ongoing refresher training, and specialized training when systems are updated. Staff should be able to explain how technology works, interpret alerts and recommendations, and troubleshoot basic issues. Ask about training frequency and methods during your evaluation.
Conclusion
AI and technology integration in assisted living communities: 2026 innovations for better care represent a significant advancement in senior care services, offering enhanced safety, personalized care, and improved quality of life for residents. From smart sensors that detect falls instantly to predictive AI that identifies health concerns before they become emergencies, these innovations provide powerful tools that support both residents and caregivers.
However, technology is only as valuable as the people who use it. The best assisted living residences combine cutting-edge innovations with compassionate, skilled caregivers who treat residents with dignity and respect. When evaluating facilities for your loved one, look for communities that use technology to enhance human connection, not replace it—where sensors and AI support care teams in providing more responsive, personalized attention.
Your next steps:
- Create your priority list – Determine which technology features matter most for your loved one’s specific health needs, safety concerns, and preferences
- Schedule tours – Visit multiple facilities to see technology in action, ask detailed questions, and observe how staff actually use systems
- Request demonstrations – Don’t just hear about technology—see it working and ask current residents about their experiences
- Review privacy policies – Carefully read consent forms and data use policies to ensure your loved one’s information will be protected
- Consider trial stays – Many facilities offer trial stay programs that let your loved one experience technology-enhanced care firsthand before committing
- Involve your loved one – Include them in facility tours and technology demonstrations so they feel empowered in the decision-making process
- Consult healthcare providers – Discuss technology options with your loved one’s physician to understand which features would be most beneficial for their specific conditions
- Compare total costs – Look beyond monthly fees to consider the value of reduced hospitalizations, better health outcomes, and family peace of mind
The transition to assisted living is a significant decision for your family. Technology can make this transition smoother, safer, and more transparent, providing the peace of mind that comes from knowing your loved one is receiving attentive, personalized care in a safe and secure environment. By choosing a community that thoughtfully integrates AI and technology while maintaining the human touch that makes assisted living truly feel like home, you’re investing in your loved one’s health, safety, and dignity.
For additional guidance on selecting the right assisted living residence, explore our comprehensive resources on emergency medical response protocols, resident satisfaction metrics, and administrator duties to understand how quality facilities operate and what standards you should expect.
Remember, the goal isn’t to find the most technologically advanced facility—it’s to find the right community where your loved one will thrive, supported by both innovative tools and caring people who are committed to helping them age with dignity.


